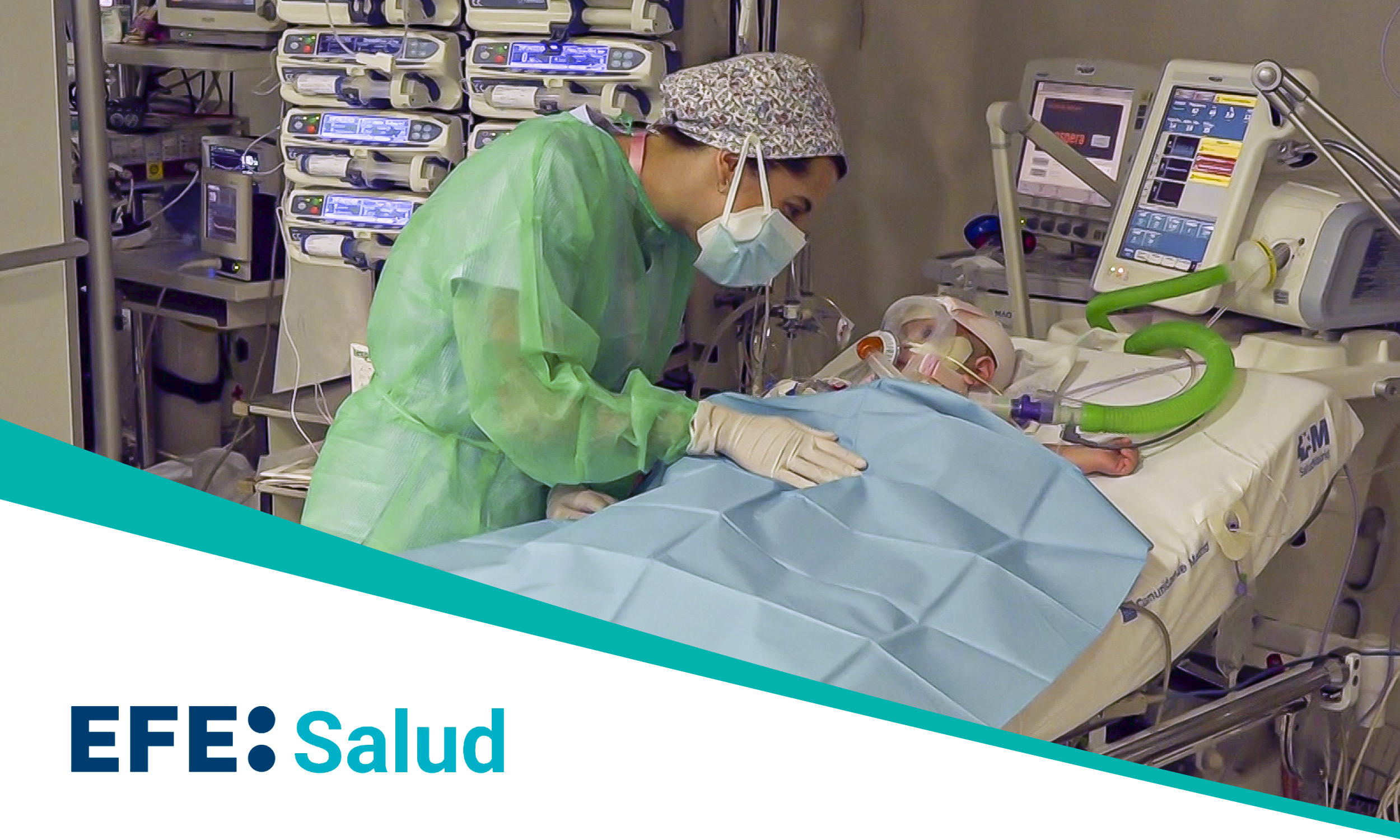
Researchers at Hospital General Universitario Gregorio Marañón have fully developed a treatment unique worldwide based on cell therapy to prevent immune rejection and potentially extend the survival of transplanted organs indefinitely, thereby prolonging patients’ lives.
The therapy and technology created by the hospital’s Immunoregulation Laboratory could establish a new paradigm in the treatment of multiple severe diseases, the Madrid-based public hospital reports.
Organ transplantation remains one of medicine’s greatest achievements. However, it is not yet a definitive solution, as immune rejection of the transplanted organ can threaten the patient’s life. In children, the limited viability of transplanted organs means life expectancy often falls short of that of healthy peers, since over time the organ may ultimately be rejected.
Six Years of Research at Gregorio Marañón
In recent years, scientific studies have demonstrated that the immune system possesses an intrinsic regulatory or tolerance mechanism mediated by regulatory T cells (Tregs), which control and reduce inappropriate inflammatory responses.
Various centers worldwide have attempted to harness these properties by developing cell therapies using Tregs obtained from patients’ blood.
Over the past six years, the Immunoregulation Laboratory at Hospital Gregorio Marañón, led by Rafael Correa Rocha, has investigated how to obtain large quantities of high-quality Tregs from an alternative source to blood.
Research conducted by Esther Bernaldo de Quirós, Marjorie Pion, and the rest of the team has led to a completely new strategy for manufacturing therapeutic doses of Treg cells from the thymus — a tissue that covers the heart and is routinely discarded during pediatric cardiac surgery.
Tregs derived from thymic tissue (thyTregs) possess unique properties and exceptionally high regulatory capacity.
First Global Trial of Treg Therapy in Children
This group is pioneering the therapeutic use of thyTreg cells in patients. In collaboration with the Pediatric Heart Unit and the Cell Production Unit of the Gregorio Marañón Health Research Institute, the team has launched a clinical trial of thyTreg cell therapy to prevent rejection in children undergoing heart transplantation.
This trial is the first worldwide to administer Treg therapy in transplanted children and, notably, the first to use thymus-derived thyTreg cells in humans instead of blood-derived Tregs. This approach enables the use of a significantly higher number of cells of superior quality, making advanced cell therapy feasible in pediatric patients.
Because the therapy uses the patient’s own cells, side effects are minimal, and it could be implemented in the near future to improve transplant survival rates.
Irene, the First Patient
Of the three children currently receiving treatment, the first was six-month-old Irene, who was born with a congenital heart condition requiring heart transplantation. She became the first patient worldwide to receive this innovative therapy following her transplant at Gregorio Marañón.
Irene is progressing favorably in her immune response, and researchers are closely evaluating how thyTreg therapy may reduce the risk of rejecting her new heart, particularly during the first post-transplant year — the most critical period.
In the months following therapy, Irene has shown higher levels of circulating Treg cells than typically observed in similar patients who did not receive cell therapy. These cells appear to be keeping inflammatory mechanisms and immune cell proliferation that could trigger rejection under control.
Expert Assessment
“We are witnessing an unprecedented medical advance that could establish a new paradigm in the treatment of various severe diseases,” explains Dr. Rafael Correa Rocha, Director of the Immunoregulation Laboratory.
“In the era of advanced cell therapies that are radically transforming cancer prognosis, our therapy harnesses and enhances intrinsic immune mechanisms to restore immune tolerance without the use of drugs,” he adds.
“We firmly believe this therapy could represent a true revolution and enable effective treatment of serious conditions such as transplant rejection, autoimmune diseases, Crohn’s disease, graft-versus-host disease, and even hyperinflammatory processes responsible for mortality in severe COVID-19 patients — positioning our country at the forefront of this major clinical breakthrough.”
Support from the Spanish National Transplant Organization
The entire process — from preclinical research to therapeutic use in patients — has been developed entirely by the Immunoregulation Laboratory at Gregorio Marañón, with financial support from the Instituto de Salud Carlos III and the Fundación Familia Alonso.
The project is also conducted under the auspices of the Organización Nacional de Trasplantes (ONT), which supports research initiatives aimed at improving Spain’s transplant system.
“What characterizes the Spanish donation and transplant system is its commitment to innovation — not only to increase organ availability, but also to improve post-transplant outcomes in terms of survival and quality of life,” says ONT Director General Beatriz Domínguez-Gil.
“The induction of immune tolerance — enabling the transplanted organ to integrate with the recipient’s immune system — is a key research priority. We are grateful for the efforts of Dr. Correa’s team in advancing this highly promising line of research. Our goal is a future with little or no immunosuppression, eliminating the burden of chronic side effects,” she adds.
International Recognition
The significance of this medical advance has also been recognized by leading international experts, including Professor Lori West, Scientific Director of the Canadian Donation and Transplantation Research Program.
“At Hospital Gregorio Marañón, they have developed a new therapy that leverages the immaturity of the pediatric immune system to provide an effective alternative to medications typically required to prevent transplant rejection. Specialized immune cells obtained from the baby can serve as a natural prevention strategy against rejection,” Professor West highlights.
More info: efesalud.com