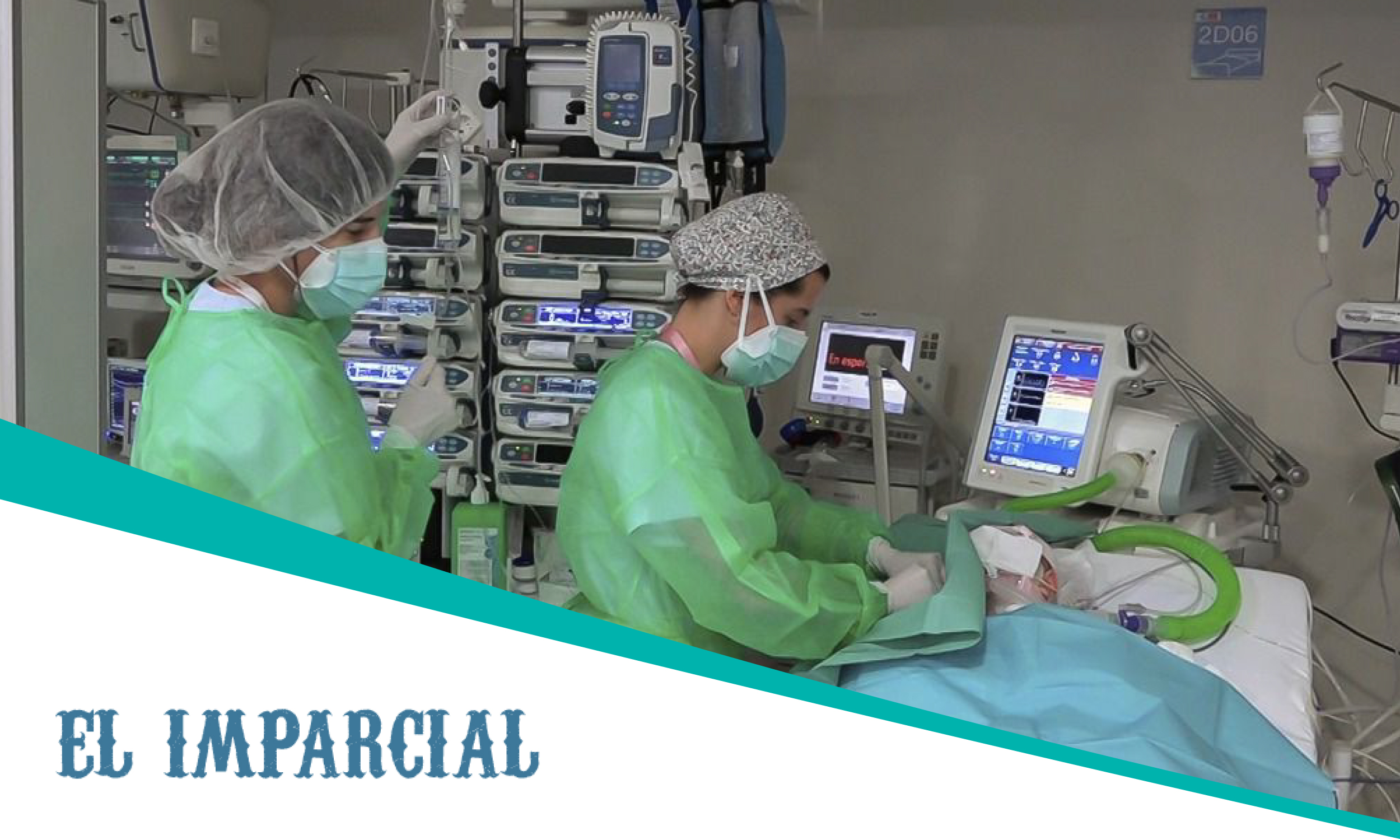
Most transplanted organs last fewer than 20 years and, therefore, are not lifelong solutions. In an effort to extend graft survival, Hospital General Universitario Gregorio Marañón has conducted research that has yielded promising results.
To make transplanted organs last a lifetime, a team at the Madrid hospital has developed a new therapy aimed at reducing the risk of rejection. By using regulatory T cells — which maintain immune balance and promote immunological tolerance — the team has been able to prevent inappropriate immune responses following organ transplantation.
Regulatory T cells are already used in adult liver and kidney transplant recipients, typically extracted from the patient’s blood. However, this approach is less effective in children because of the large blood volumes required. “That’s why, instead of looking for regulatory cells in the blood, we turned to the thymus — a primary lymphoid organ located near the heart — as a source of regulatory T cells,” explained Rafael Correa, Head of the hospital’s Immunoregulation Laboratory.
The thymus is relatively large during childhood but shrinks during adolescence and tends to disappear in adulthood.
“We recover the thymus tissue that is removed during surgery and isolate regulatory cells from it,” Correa continued. The advantage is significant: around two million regulatory cells can be obtained from a child’s blood, or about 30 million from an adult’s blood, whereas up to ten billion cells can be extracted from a child’s thymus. In addition, thymus-derived cells have longer persistence and greater regulatory capacity than those obtained from blood.
Researchers report that three infants who have undergone heart transplantation are already being treated with this technique and are progressing favorably. Nine months after starting therapy, the first patient continues to show no signs of rejection and maintains adequate levels of regulatory cells — a key factor in preventing rejection.
“Although these are preliminary results, they are highly encouraging. We believe this could open a new era in the clinical management of immune rejection. Thanks to this therapy, we hope she will be able to keep her new heart for many years,” Correa stated.
He noted that half of pediatric heart transplants fail before 15 years. Currently, immunosuppressive drugs are used to prevent rejection, but they have significant drawbacks. “They are not entirely effective at preventing rejection, and treated children have a higher incidence of autoimmune diseases or cancer,” he explained.
This clinical trial is supported by the Organización Nacional de Trasplantes (ONT) and Canada’s transplant program.
It is the first trial worldwide to apply thymus-derived regulatory T cell therapy in transplanted children. By obtaining a greater number of higher-quality cells, the therapy becomes feasible in pediatric patients.
This new approach may restore proper immune balance and could completely inhibit or significantly reduce immune responses responsible for rejection, potentially allowing indefinite survival of the transplanted organ — and thus extending the patient’s life. Because it uses the patient’s own cells, side effects are minimal, and the therapy could be implemented in Spanish hospitals in the near future, further improving transplant outcomes in a country that leads the world in organ donation and transplantation.
More info: elimparcial.es